FAT CONTAINING LESIONS OF THE BONES:
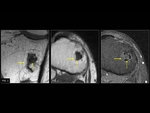
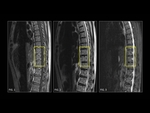
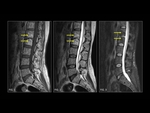
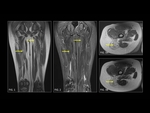
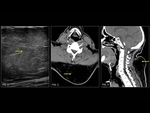
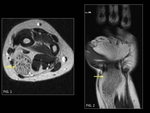
Intraosseous lipomas (Fig. 1) were first described in 1880.
The lesions typically affect patients in age from 5 to 85 years,
with the lesions frequently discovered in the 4th and 5th decades of life.
Intraosseous lipomas have been reported to occur in equal frequency in both genders.
Patients are generally asymptomatic.
And lesions are discovered incidentally.
Uncommonly pain may be the presenting feature and is thought to be due to microtrabecular fractures occurring after minor trauma in the weakened bone.
Milgram has proposed 3 stages in the evolution of intraosseous lipomas.
Stage 1: Radiolucent expansile lesion with viable lipocytes and some fine bone trabeculae on histology.
Stage 2: Lesions are radiologically like stage 1 lesion,
but partial fat necrosis and focal calcification with regions of viable lipocytes are seen on histology.
Stage 3: Radiologically it shows a reactive ossified rim,
some central cysts and calcification correlating with complete fat necrosis during histological examination.
Computerized Tomography demonstrates an area of low attenuation of fat (<–60 to –100 HU) and MRI shows T1 prolongation and T2 shortening like subcutaneous fat.
.
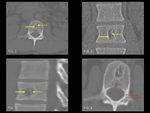
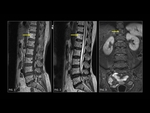
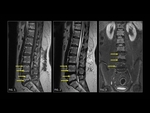
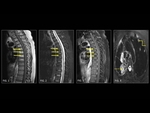
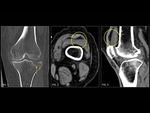
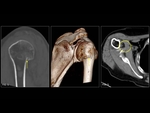
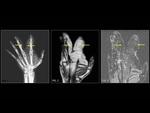
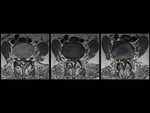
Intraosseous hemangiomas (Fig. 2,
Fig. 3) are benign vascular tumors.
Vertebral body hemangiomas are the most common tumors of the spine.
They account for 10-20% of spine tumors in adults.
The most common site is the thoracolumbar spine.
Most hemangiomas are painless and asymptomatic,
detected only incidentally.
There is no gender preponderance.
Approximately 20-30% of hemangiomas are multifocal and may vary from Subcentimeter in size to replacing the entire vertebral body.
They are often limited to the vertebral body,
but few may extend into the posterior elements.
Osseous hemangiomas are actually slow growing hamartomas.
Histopathologically they consist of thin-walled blood vessels and sinuses lined by endothelium and interspersed among sparse longitudinally oriented trabeculae of bones.
The dilated vascular channels are set in a stroma of fat.
Hemangiomas have typical appearances on CT and MR.
At CT,
hemangiomas have a vertically striated appearance due to thickening of bony trabeculae.
This is described as “corduroy cloth” or “jail bar” appearance and the overall density of the vertebral body is decreased due to the presence of fatty marrow. On an axial scan,
the presence of a haemangioma imparts the “salt and pepper” or “polka dot” appearance.
At MRI,
the intralesional fat of the hemangioma causes increased signal intensity on T1W and t2W images.
On T2-weighted images,
the signal intensity of the hemangiomas also increases because of high water content to the extent that the signal intensity is typically greater than that of fat,
thus differentiating hemangiomas from focal fat deposition.
The signal intensities of atypical hemangiomas can be indeterminate,
but the morphology of the lesion,
including the presence of coarse trabeculae,
can be used to make the diagnosis.
.
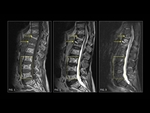
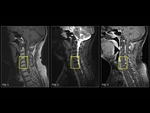
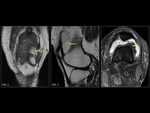
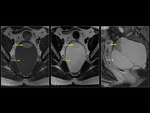
At MRI,
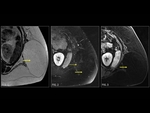
osteoporosis (Fig. 4) can have a heterogeneous,
more commonly a variegated appearance.
This occurs due to decreased cellular marrow components and increased fat content.
T1W images show heterogeneously hyperintense signal intensity,
scattered throughout the spine.
The T2W signal can be variable.
STIR imaging in cases of osteoporosis of the spine particularly helps in identifying fracture related marrow edema.
Another added benefit of obtained STIR images is the identification of multiple myeloma.
The disease tends to cause diffuse osteopenia,
which on convention non-fat suppressed pin echo sequences is indistinguishable from osteoporosis.
Punctate STIR hyperintensities in these cases represent myelomatous deposits (Fig. 5).
.
Degenerative endplate changes (Fig. 6) were described by Modic et al.
In their original research paper,
they examined histopathologic of the spine and classified degeneration into three categories.
Type 1 changes were edematous marrow lesions caused due to disruption and fissuring of endplates and formation of a fibrovascular granulation tissue.
Type 2 changes were associated with fatty degeneration of the red marrow and its replacement by yellow marrow,
causing high signal intensity on T1W and T2W images.
A third type,
type 3,
was subsequently added which represented end-stage changes of sclerosis.
In summary,
type 1 changes correspond to the active inflammatory stage of degeneration,
whereas type 2 changes represent the fatty,
more stable stage of degeneration.
.
Radiotherapy-related marrow changes (Fig. 7) are time and dose-dependent.
The acute phase post-irradiation (day 1–3),
the marrow develops edema,
which appears hypointense on T1W and hyperintense on fat-saturated T2W and STIR images.
Gadolinium administration may reveal a transient enhancement during this phase.
The bone marrow ultimately undergoes a fatty conversion,
which closely follows the irradiation field.
Marrow at this time appears follows the signal intensity of subcutaneous tissues.
Depending on the applied dose,
the fat marrow conversion may be detected as early as 10–14 days following therapeutic irradiation.
Fatty conversion is reversible after irradiation of less than 30–40 Gy and irreversible after an irradiation with more than 40 Gy.
.
Chemotherapy (Fig. 8, Fig. 9),
particularly in patients with leukemia,
results in typical signal changes of the bone marrow on MR images.
These reflect the underlying changes in the cellular composition and vascularity of the bone marrow.
During the first week of therapy,
the marrow sinus becomes dilated and hyperpermeable,
leading to edema.
Subsequently,
a marked decrease in bone marrow cellularity and a fatty conversion of the bone marrow ensues,
characterized by marrow hyperintensity on T1W and T2W images,
suppressed on fat saturation.
After successful therapy,
a normalization of the MR signal occurs with regeneration of normal hematopoietic cells in the bone marrow.
.
FAT CONTAINING LESIONS OF THE MUSCLES:
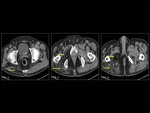
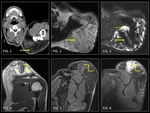
Lipomas (Fig. 10) are the most common type of soft tissue mesenchymal tumors.
Infrequently,
they may arise within a muscle and are called intramuscular lipomas (ILs).
ILs are relatively uncommon and accounts for about 1.8% of all primary tumors of adipose tissue and less than 1% of all lipomas.
They may occur in all age groups,
from childhood to old age,
though the majority occur between the ages of 40 and 70 years.
Reactive pathogenesis has proposed in the development of this tumor.
Some of the plausible etiologies include trauma,
chronic irritation,
obesity,
developmental disorders,
endocrine,
dysmetabolic and genetic factors provoking the uncontrolled growth of lipomas.
Pathologically they contain adipocytes of uniform size and shape which irregularly infiltrate between muscle fibres.
These may also completely replacing the muscle bundles.
A result of this lead to the appearance at CT scans and MRIs.
Rarely the tumors may undergo necrosis,
which may impart hyperintense signals on fluid-sensitive imaging techniques
.
Muscle denervation (Fig. 11) results from a variety of causes including trauma,
neoplasia,
neuropathies,
infections,
autoimmune processes and vasculitis.
Traditionally electromyography was used in the identification of these injuries,
however,
with the advent of MRI,
there has been a shift in the modality of investigation.
Magnetic resonance imaging (MRI) helps in identifying the stage of denervation as well as often can also help in identifying the cause.
The acute and subacute phases of denervated muscles show a hyperintense signal on fluid-sensitive sequences and normal signal intensity on T1-weighted MRI images.
In chronic denervation,
muscle atrophy and fatty infiltration demonstrate high signal changes on T1-weighted sequences in association with volume loss.
Fatty infiltration due to chronic denervation is usually accompanied by muscle atrophy and represents irreversible muscle injury.
.
Muscle atrophy with fatty infiltration (Fig. 12) may be also be seen in non-neurologic conditions.
These usually mimic chronic denervation on MR images.
Chronic muscle disuse,
e.g.
following prolonged cast immobilization,
leads to atrophy with fatty infiltration.
At CT / MRI a search of potential non-neurological causes of such atrophy,
e.g.
tendon rupture,
old healed fractures,
osteoarthritis etc,
must be performed to avoid misinterpretation as Muscle denervation.
.
Duchenne muscular dystrophy (DMD) (Fig. 13) is one of the most common neuromuscular disorders in children.
It is a fatal X-linked recessive dystrophy with an incidence of one in 3500 boys.
DMD is caused due to a mutation or absence of dystrophin,
which otherwise forms a membrane-bound glycoprotein complex in muscle tissue that helps maintain plasma membrane integrity.
The absence of this causes instability of plasma membranes and makes the muscle fragile and susceptible to injury during concentric contraction.
Muscle injury,
repair,
and inflammatory changes in the early phases followed by a progressive,
irreversible fatty infiltration.
.
FAT CONTAINING LESIONS OF THE JOINTS:
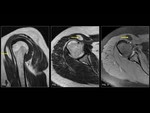
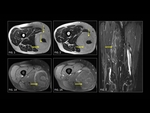
Lipohemarthrosis (Fig. 14, Fig. 15) is defined as the presence of free-floating fat within a joint cavity with a dependent layering of blood and fluid.
Traumatic injury represents the most common cause,
and lipohemarthrosis is widely considered pathognomonic of an acute fracture.
It occurs secondary to an intraarticular fracture and is an important diagnostic clue to the identification of a fracture.
.
Lipoma arborescens (Fig. 16) is a lipoma associated with the synovial lining of a joint or soft-tissue structure.
It is most likely a reactive process,
although other postulated causes include posttraumatic,
developmental,
and neoplastic etiologies.
Histologically it is characterized by mature fatty infiltration of connective tissue just below the synovial lining.
It commonly manifests in adults with gradual joint swelling.
Pain is uncommon.
The most commonly affected joint is the knee joint particularly the suprapatellar recess.
Most cases are monoarticular,
with rare polyarticular involvement.
Cases of extra-articular lipoma arborescens have been reported,
involving the peroneal and flexor ankle tendon sheath,
subdeltoid bursa,
extensor tendon sheath of the hand,
and biceps tendon sheath.
The condition is best diagnosed at MRI.
It is characterized by a frondlike,
lobulated fat-containing tissue within the joint space and is usually associated with joint effusionS.
Advanced cases may show findings of subchondral erosions,
subchondral cysts,
or secondary osteoarthritis.
.
FAT CONTAINING LESIONS OF THE SUBCUTANEOUS TISSUES:
Subcutaneous lipoma (Fig. 17,
Fig. 18) account for almost 50% all soft-tissue tumors.
It is the most common subcutaneous neoplasm.
Lipomas occur most commonly between the 5th to 7th decades of life and are more common in obese patients.
Most lesions show heterogeneous balanced structural chromosomal aberrations,
most involving a breakpoint in the chromosomal region 12q13-15,
resulting in expression of truncated HMGA2 protein or a fusion protein.
Pathologically,
lipomas are composed of homogeneous mature adipose tissue.
Lipomas are categorized as superficial or deep based on their location relative to the fascia overlying the deep muscles.
Lipomas may be encapsulated or unencapsulated and may contain non-adipose tissue like fibrous tissue,
cartilage,
bone,
and myxoid tissue,
which can mimic other tumors (Fig. 19).
Lipomas typically resemble subcutaneous fat on CT scans and MRI but may contain a few thin septa measuring less than 2 mm in thickness which may enhance following contrast administration.
.
Hibernoma (Fig. 20) is an uncommon benign tumor of brown fat usually manifesting in adults as a painless,
slow-growing mass.
These are well-circumscribed,
partially encapsulated hypervascular masses.
Four histologic variants have been described: typical hibernoma,
lipoma-like variant,
myxoid variant,
and spindle cell variant.
Most hibernomas are positive for S100 and most,
except spindle cell variant,
are negative for CD34.
Hibernomas may show 11q13 and 11q21 chromosomal rearrangements.
Hibernomas are fat-containing lesion but are associated with prominent vascularity and septa.
At MRI,
these tumors appears well-defined with T1 signal characteristics that is greater than that of skeletal muscle but less than that of subcutaneous fat.
The lesion may fail to completely suppress on fat-saturation and may demonstrate heterogenous hyperintensity on fluid-sensitive images.
They tend to show hypermetabolic activity at PET/CT.
Surgical resection is almost always curative.
.
FAT CONTAINING LESIONS OF THE NERVES:
Lipomatosis of nerve (LN) (Fig. 21) also known as fibrolipomatous hamartoma is a benign poorly understood condition.LNs commonly occurs in the wrist and hand,
along the median nerve and its branches,
though it has been reported in multiple other distributions,
including the ulnar,
radial,
digital,
sciatic,
intercostal,
and medial plantar nerves as well as the cervical,
brachial,
and lumbosacral plexus.
Pathologically,
LN features diffuse nerve enlargement secondary to interfascicular fibrofatty infiltration.
The intervening nerve fibres are intact.
The growth continues after skeletal maturation but usually slows down in late adulthood.
LNs can involve single or multiple nerves in an extremity and can be unilateral or bilateral,
usually presenting as a painless,
slowly enlarging mass.
LN is frequently associated with varying degrees of localized mesenchymal overgrowth in the territory of nerve distribution.
This ranges from minimal digital enlargement to extensive bone and soft-tissue hypertrophy,
referred to as macrodystrophia lipomatosa (Fig. 22).
The MR imaging findings of diffuse nerve enlargement with T1-hyperintense fat interspersed between normal T1-hypointense nerve fascicles are pathognomonic.
There is no curative treatment available for this disease.
The goal of surgery includes symptomatic relief and cosmetic and functional improvement of the deformity.
.
Fatty filum terminale,
or lipoma of the filum terminale or filar lipoma (), is a commonly encountered finding in MR imaging of the lumbar spine.
These are generic terms which imply a fibrolipoma within the filum histologically.
Theoretically,
they develop during the latter stage of canalization and differentiation.
A fibrolipoma “infiltrates” the filum and tends to be tubular as opposed to a dural lipoma.
These are often incidentally picked up and usually present with no clinical concern.
In some patients,
however,
they may be associated with tethered cord syndrome.
In such cases,
it is associated with a thickened filum and a low-lying conus.
.
INCIDENTALLY DETECTED FAT CONTAINING LESIONS:
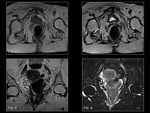
Germ cell tumors (Fig. 24) occur secondary to disorganization of totipotent primitive neural cells during embryogenesis.
The degree of differentiation determines the tumor type and its malignant potential.
Sacrococcygeal teratoma is the most common presacral germ cell tumor in children and the most common solid tumor in neonates.
Isolated presacral teratomas in adults are rare and possibly only a few have been reported in the medical literature.
The imaging features of teratomas depend on their contents.
Benign teratomas contain only mature tissues,
including fluid,
fat,
calcification,
and a small amount of soft tissue.
This leads to a mixed but well distinguishable attenuation and signal intensity on CT and MR imaging respectively.
Malignant tumors have more solid tissue than benign tumors,
with areas of hemorrhage and necrosis common.