Keywords:
Education and training, Imaging sequences, CT, Respiratory system
Authors:
R. Pothera1, C. P. Mathew2, A. V. Nair3, S. K. Pullara1, D. Viswam1, S. Moorthy1; 1Kochi/IN, 2Kochi, Ke/IN, 3Trivandrum, kerala/IN
Results
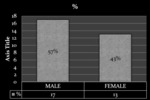
Fig-5: Study population

Fig. 5: Study population
- In this study,
consisting of 30 IPF patients,
13 were female (43%),
and 17 were male(57%)
- Mean ageof the study sample was 60.7.
Fig-6: Study population- Age distribution

Fig. 6: Study population- Age distribution
Table-1 : HRCT findings in the 30 patients with IPF.
|
HRCT findings
|
Affected patients
|
%
|
|
Reticular abnormality
|
30
|
100
|
|
Honeycombing
|
26
|
86
|
|
Honeycombing ,
Cysts ↓3mm
|
26
|
86
|
|
Honeycombing ,
Cysts ↑3mm
|
13
|
43
|
|
Traction bronchiectasis
|
29
|
96
|
|
Associated significant emphysema
|
7
|
23
|
- Peripheral distribution /sub pleural predominance of lesions seen in all patients.
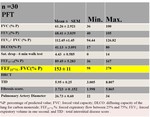
Table-2: Mean of physiological indices and HRCT findings

Table 2: Mean of physiological indices and HRCT findings
(FVC: forced vital capacity; DLCO: diffusing capacity of the lung for carbon monoxide; FEF25-75 %: forced expiratory flow between 25% and 75%; FEV1: forced expiratory volume in one second; and TID: total interstitial disease score .)
- The higher ratio suggests increased elastic force exerted by the connective tissue abnormally deposited in the parenchyma,
keeping airways open.
- In our study group and in the studies of Lopes et al the TID scores correlated positively with FEF25-75 / FVC
Table 3.
Correlations between HRCT findings & functional indices.

Table 3: Correlations between HRCT findings & functional indices.
(FVC: forced vital capacity; DLCO: diffusing capacity of the lung for carbon monoxide; FEF25-75 %: forced expiratory flow between 25% and 75%; FEV1: forced expiratory volume in one second; and TID: total interstitial disease score .)
- Karl Pearson coefficient of correlation was used to examine the correlation in the total study group.
- **.
Correlation (Corr.) is significant at the 0.01 level.
- Strongest correlation was observed between TID and percentage of predicted DLCO (negative correlation) (p = 0.001).
- No correlation was observed between either the fibrotic score or pulmonary artery diameter (P.A.) and the functional indices.
Table 4.
Correlations between HRCT findings & functional indices.

Table 4: Correlations between HRCT findings & functional indices.
(FVC: forced vital capacity; DLCO: diffusing capacity of the lung for carbon monoxide; FEF25-75 %: forced expiratory flow between 25% and 75%; FEV1: forced expiratory volume in one second; and TID: total interstitial disease score)
- Karl Pearson coefficient of correlation was used to examine the correlation in the total study group
- **.
Correlation (Corr.) is significant at the 0.01 level.
- Strongest correlation was observed between TID and percentage of predicted DLCO (negative correlation) (p = 0.001).
- No correlation was observed between either the fibrotic score or pulmonary artery diameter (P.A.) and the functional indices.
Table 5.Correlation in the group having no emphysema

Table 5: Correlation in the group having no emphysema
- Analyzed using Spearman’s rank correlation.
- When patients with significant emphysematous changes were excluded,
negative correlation between FVC and TID was observed.
Table 6. Comparison of the overall lung involvement based on DLCO using Independent sample t test

Table 6: Comparison of the overall lung involvement based on DLCO using Independent sample t test
- After grouping into advanced disease and limited disease based on DLCO17,18,19 (DLCO<39 / DLCO> 40) The two-tailed t test was used to compare the average of TID scores .
- Significant difference was noted in TID values of both groups.
- Correlation is significant at the 0.05 level .
Fig-7: ROC curve

Fig. 7: ROC curve
- From the ROC curve plotted based on the data ,
we found that a cut off value of six could separate the patients with advanced disease with a sensitivity of 85% and specificity of 65%.
Study Limitations
- In the sample evaluated,
surgical biopsy was not performed,
requiring that clinical,
radiological and functional parameters be adopted as inclusion / exclusion criteria.
- Another limitation was the use of semiquantitative scores to evaluate the extent of abnormalities on HRCT scans,
although previous studies showed a perfectly acceptable degree of interobserver variation(Collins et al).