We included 199 trainees and fellows with an interest in thoracic and cardiovascular imaging (79 females; 4 did not reveal their gender.
137 (69%) participants were residents in European countries; 138 of participants did core training in Europe.
See Figures 1-6 and Tables 1-7.
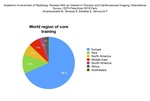
Geographical distribution is displayed in Fig. 1.
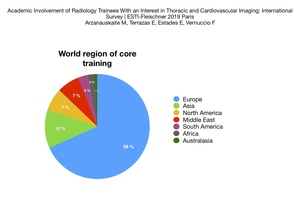
Fig. 1: Participant distribution in world regions Africa (Ethiopia 1, Morocco 1, Tunisia 1), Asia (India 5, Philippines 10, Russia 1, Singapore 1, South Korea 5, Thailand 2), Australasia (Australia 1), Europe (Austria 1, Belgium 10, Bulgaria 1, Croatia 2, Czech Republic 1, Denmark 6, France 1, Germany 2, Greece 4, Hungary 1, Italy 74, Lithuania 17, Netherlands 1, Norway 1, Portugal 1, Serbia 1, Spain 2, Switzerland 3, UK 9), Middle East (Bahrain 1, Egypt 7, Lebanon 1, Saudi Arabia 1, Turkey 4), North America (Mexico 6, USA 8), South America (Argentina 5)
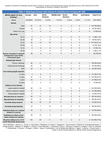
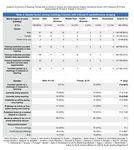
Table 1 covers values distributed by world regions as well as total numbers on: age groups,
academic background in family,
subspecialty interest,
setting of core training,
allocated time for academic activities,
current academic activities,
publications and willingness to do a fellowship.
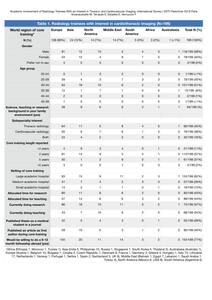
Table 1: Radiology trainees with interest in cardiothoracic imaging. Distributed by world regions as well as total values on: age groups, academic background in family, subspecialty interest, setting of core training, allocated time for academic activities, current academic activities, publications and willingness to do a fellowship.
Gender factor
Although no significant differences were recorded in terms of documented research involvement (presentations in meetings/publications) between females and males,
a significantly higher number of females (22/79,
28%) consider their gender as a challenge in academic opportunities compared to males (8 of 116,
7%) (p<0.002), Table 2, Fig. 2.
A significantly higher number of male participants were involved in teaching activities (50/116,
43%) (p<0.02).
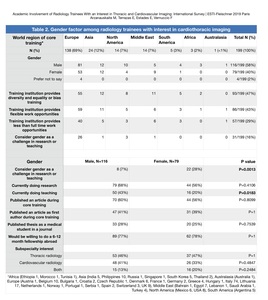
Table 2: Gender factor: equality and diversity training, flexible work opportunities, less than full work time opportunities, perceived gender barrier, publications, willingness to do a fellowship, subspecialty interest. Data plotted in world regions and/or gender groups.
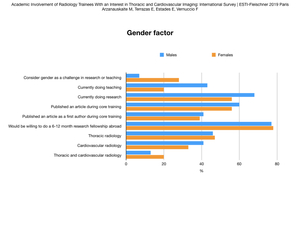
Fig. 2: Gender factor distributed by male and female groups
Attitude factor
Only a small number of trainees think research practice may compromise clinical competency (22/199,
11%).
However,
the majority (130/199,
65%) think research practice improves clinical competency,
and 91/199 (46%) are of opinion that research practice should be included in any radiology training program.
Similarly,
137/199 (69%) believe teaching practice improves clinical competency,
and 43% think teaching practice should be included in any radiology training program.
See Table 3 and Fig. 3.
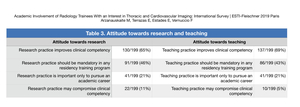
Table 3: Attitude towards research and teaching
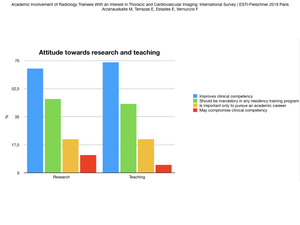
Fig. 3: Attitude towards research and teaching
Barriers
The most important reported barriers limiting involvement of residents in research activities were: lack of time (128/199,
64%),
lack of research mentorship (49%) and lack of support from faculty / senior radiologist (42%).
The most important reported barriers limiting involvement of residents in teaching activities were: lack of time (128/199,
57%),
lack of support from faculty/senior radiologist (40%) and lack of teaching mentorship (38%).
See Table 4.
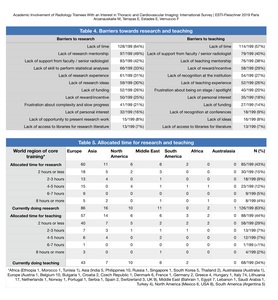
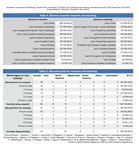
Table 4: Table 4. Barriers limiting involvement of residents in research activities.
Table 5. Detailed allocated time for research and teaching.
Time factor
126/199 (63%) trainees are currently doing research.
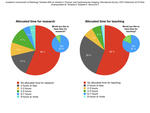
85/199 (43%) trainees had formally allocated time for research; 71/85 (84%) reported ≤ 5 hours per week (Table 4).
Among those who did not have formally allocated time for research,
110/122 (90%) would like to have it.
68/199 (34%) trainees are currently doing teaching.
88/199 (44%) trainees had allocated time for teaching; 83/88 (94%) reported ≤ 5 hours per week.
Among those who did not have formally allocated time for teaching activities,
101/124 (81%) would like to have it. See Fig. 4.
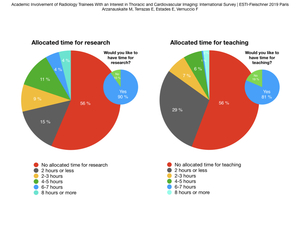
Fig. 4: Protected time for research and teaching
Interest in further training
154/199 (77%) of trainees would be willing to do a research fellowship abroad.
Among the main barriers for such fellowships,
144/199 (72%) report lack of funding and a possible reduction of overall income.
See Fig. 5.
Among the trainees (44/199,
22%) who would not be willing to do a research fellowship,
22/44 (50%) report lack of interest,
and 18/44 (41%) do not see future possibilities after doing research.

Fig. 5: Table 6. Publications during core training.
Table 7. Top reasons for not pursuing a research fellowship after core training.
Future work setting
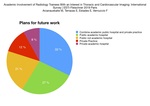
The vast majority of trainees are planning to work in academic environment (133/199,
67%).
In this group,
64/199 (32%) would combine academic public hospital and private practice,
53/199 (27%) are planning to work in a public academic hospital,
and 16/199 (8%) are planning to work in a private academic hospital.
Meanwhile,
42/199 (21%) participants are planning to work in a public not academic hospital.
Only 24/199 (12%) participants are planning to work in private (not academic) practice.
See Fig. 6.
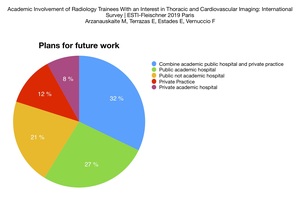
Fig. 6: Plans for future work: academic/not academic and private/public setting