The concept of Size-Specific Dose Estimates (SSDE) for refining computed tomography (CT) dosimetry has been proposed in the Report of the American Association of Physicists in Medicine (AAPM) Task Group 204.[1] The present conventional metrics for determining patient exposure in CT applications are the volume Computed Tomography Dose Index (CTDIvol) and Dose Length Product (DLP),
which do not take patient size into account.
Tube current modulation (TCM) functionality is used in most CT examinations to achieve consistent clinical image quality independent of patient size,
resulting in a natural scatter in CTDIvol and DLP,
dependent on patient size.
Clinical audit and optimization work is thus not straightforward using the CTDIvol and DLP metrics.
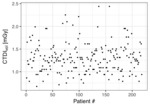
See Fig.
1 for example of CTDIvol scatter for a cohort 218 of thorax CT examinations.
Estimation of the SSDE is done in two steps; first,
patient size is determined from the actual CT images,
using either the localizer radiograph(s) or axial images.
When patient size is known,
the Report of AAPM Task Group 204 supplies correction factors,
f,
tabulated per patient size,
which are used together with the CTDIvol to determine the SSDE,
i.e.
SSDE=f∙CTDIvol.
Physical patient size,
in cm,
is easily determined manually from a patient image,
e.g.
by a measurement tool in PACS.
However,
this is not feasible in large-scale optimization and clinical audit projects.
Furthermore,
as detailed in the Report of AAPM Task Group 220,
a more robust metric for estimating patient exposure via the SSDE is the water equivalent diameter (WED),
which determines patient size as equivalent thickness of X-ray beam attenuation in water.
The WED is particularly well suited for making the SSDE robust in comparisons of patient exposure between different anatomical regions,
e.g.
thorax and abdomen,
where physical patient size may be very similar but the attenuation properties varies considerably due to tissue density.
The WED cannot be determined manually from patient images,
nor is it feasible to use the less robust metric given by patient physical size in large-scale projects,
as previously discussed.
In this work we,
therefore,
present results from a software solution,
which is part of the REMbox framework (Dicom Port AB,
Umeå,
Sweden),
for determining the SSDE via automated image segmentation.
Furthermore,
when working in the image domain other quality assurance related metrics can be determined,
e.g.
evaluation of patient centring in CT examinations.
Patient centring in CT has been discussed for a long time from an optimization and quality assurance perspective,
due to complex relations between bow-tie filter X-ray beam shaping and TCM.
Optimal functionality with regard to both clinical image quality and patient exposure should be achieved if the patient is perfectly centred in the CT gantry.