Purpose or learning objective
1) To audit the awareness of radiation risks amongst junior doctors at a small UK district general hospital (Diana Princess of Wales Hospital, Grimsby, UK).
2) To assess the effectivness of a pre-recorded online teaching session on radiation exposure and risks of malignancy of commonly preformed radiological investigation in improving junior doctors' knowledge in these topics
Methods or background
Radiological investigations have become essential tools in modern clinical practice to confirm diagnoses and to monitor responses interventions. Some of the most commonly performed radiological investigations by junior doctors from medical and surgical specialties involve CXR, AXR, CT Chest, CT Abdomen and Pelvis, CT KUB and CT head.
With the increased utilisation of medical imaging, it has become important for referring clinicians to be aware of the potential harms associated with ionising radiation in the interest of patient safety and to avoid unnecessary exposure. Cumulative...
Results or findings
1) Response rate = 52% (n=16)
2) 38.4% of respondents = women, 61.6% = men
3) 60% of respondents were first year doctors, 40% were second year and above.
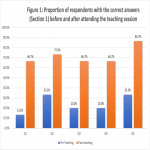
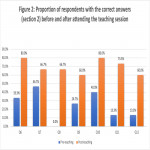
4) There are significant improvement in the proportion of correpsondents with the correct answers across the questions in both question sets after watching the pre-recorded teaching video (P value <0.05 for both question sets) as shown in Figure 2 and Figure 3.
5) Both pre-defined standards were not achieved in general.
Conclusion
Conclusion
1 ) There is a knowledge gap in radiation risk amongst junior doctors
2) Pre-recorded teaching session could be beneficial in closing this knowledge gap, and this could be a more practical way to educate junior doctors while we are still in the middle of the COVID-19 pandemic.
3) More effort is needed to further improve radiation safety awareness in junior doctors
Limitations:
1) Small sample size
2) Low response rate to the questionnaire
References
1) The Ionising Radiation (Medical Exposure) Regulations 2017http://www.legislation.gov.uk/uksi/2017/1322/introduction/made
2) S Shiralkar, A Rennie, M Snow, R B Galland, M H Lewis, K Gower-Thomas, Doctors’ knowledge of radiation exposure: questionnaire study. BMJ 2003;327:371–2.https://www.ncbi.nlm.nih.gov/pmc/articles/PMC175104/
3) J A Soye, A Paterson. A survey of awareness of radiation dose among health professionals in Northern Ireland. Br J Radiol. 2008 Sep;81(969):725-9.https://www.birpublications.org/doi/abs/10.1259/bjr/94101717
4) Awareness of radiation risks by referrers and practioners justifying radiological examinations (RCR audit live dabatase): https://www.rcr.ac.uk/audit/awareness-radiation-risks-referrers-and-practitioners-justifying-radiological-examinations
Personal information and conflict of interest
M-T. Lee:
Nothing to disclose
A. K. Ang:
Nothing to disclose
M. H. Abdi:
Nothing to disclose
J. Alex:
Nothing to disclose