Congress:
EuroSafe Imaging 2021
Keywords:
Artificial Intelligence, Molecular imaging, Radioprotection / Radiation dose, Gamma knife, Image manipulation / Reconstruction, PET-CT, Ablation procedures, Audit and standards, Chemoembolisation, Biological effects, Education and training, Quality assurance
Authors:
M.-T. Lee, A. K. Ang, M. H. Abdi, J. Alex
DOI:
10.26044/esi2021/ESI-14270
Methods or background
Radiological investigations have become essential tools in modern clinical practice to confirm diagnoses and to monitor responses interventions. Some of the most commonly performed radiological investigations by junior doctors from medical and surgical specialties involve CXR, AXR, CT Chest, CT Abdomen and Pelvis, CT KUB and CT head.
With the increased utilisation of medical imaging, it has become important for referring clinicians to be aware of the potential harms associated with ionising radiation in the interest of patient safety and to avoid unnecessary exposure. Cumulative exposure to ionising radiation can increase the probability of developing a malignancy.
The UK Ionising Radiation (Medical Exposure) Regulations 20171 encourages referrers of radiological investigations to be equipped with the knowledge of their estimated radiation doses. Junior doctors being the main requesters of most in-hospital radiological investigations should be aware of the effective radiation doses and the associated risks of malignancy of commonly performed radiological investigations. These knowledge would further ensure decisions to put patients thorugh radiological investigations would be in their best interests. Multiple previous studies have suggested that junior doctors are lacking in the knowledge required to make a informed decision (weighing up benefits of investigation against risks of radiation exposure) when requesting radiological investigations3,4.
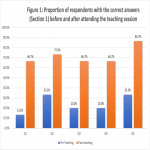
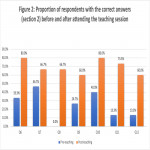
Data was collected using a survey containing 2 question sets; 5 questions testing doctors' knowledge of effective radiation dose of commonly requested investigations and 7 questions on their corresponding estimated associated total lifetime cancer risks (Figure 1). This survey was adapted from an audit template obtained from the Royal College of Radiologists' online audit database4 . This survey was then distributed to 31 pre-specialty training doctors.
A pre-recorded teaching was then distributed to the respondents. The teaching covered the following relevant areas; IR(ME)R, effective radiation doses of commonly requested scans, brief overview of radiation biology and lifetime malignancy risks associated with commonly requested scans. The same survey was then re-distributed to the same group of doctors.
Data collected in both surveys were compared against each other and also with pre-defined audit standards and analysed.
Audit Standards:
1. 80% should have knowledge of effective radiation dose of commonly investigations.
2. 80% should have knowledge of approximate added risk of malignancy of these investigations.