Keywords:
Cardiac, MR, Imaging sequences, Ischaemia / Infarction
Authors:
A. Damascelli, F. De Cobelli, A. Esposito, M. Cava, G. Benedetti, A. Durante, A. Colombo, P. G. Camici, A. Del Maschio; Milan/IT
DOI:
10.1594/ecr2013/C-1057
Results
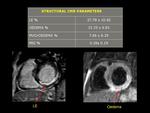
All patients showed myocardial oedema (33±9%) and LE (28±11%) at CMR.
The average EF was slightly depressed (50.19 ± 9.89) (see fig.
5 and 6)
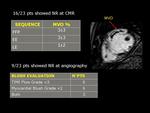
17 patients showed NR considering both CMR and coronary angiography.
In particular we observed that 16 patients showed MVO at CMR,
while only 9 patients showed MVO at coronary angiography.
Among the group of 9 patients positive for MVO at angiography one was negative at CMR.Considering MVO at CMR,
it was present on all dedicated sequences: FFP (3± 3%),
EE (3± 3%) and LE (1±2%).
(See fig.
7 and 8)
TIMI flow grade and BLUSH grade were compared with CMR findings: only TIMI grade correlated with MVO% at CMR (p=0.029).
CMR parameters were correlated with cardiac function and we found that LE% and oedema% showed inverse correlation with LVEF (p=0.004; p=0.032).
The presence of NR was inversely related to LVEF as well (p=0.027).
Among angiography parameters only TIMI flow grade correlated with LVEF (p=0.027).
Furthermore we evaluated the incidence of Major Adverse Cardiac Events (MACE) during the first 30 days after the infarction,
recording events in 3 patients: 1 cardiac death,
1 papillary rupture and one ICD implantation [4,5].
We found that patients with MACE presented a significantly higher MVO% (p=0.038).
We also observed that patients with MVO were hospitalised for a longer period than patients without MVO (P=0.007) (See fig.
9).
No angiographic parameters presented similar correlation with MACE and period of hospitalisation.