Learning objectives
Review of the anatomical course of the oculosympathetic pathway.
Discuss key anatomical and radiologically-discernible sites of pathology within thepathway.
Explanation of the most common clinical manifestation of oculosympathetic disease - Horner's syndrome.
Demonstration of specific radiological examples of pathology affecting various portions of the oculosympathetic chain.
Background
Horner’s syndrome occurs when there is disruption to the oculosympathetic pathway.
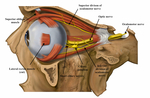
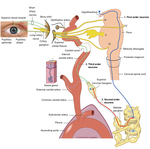
The pathway takes a circuitous route from its central origin to its distal innervation of the orbit.
Subsequently,
the pathway can be interrupted at a number of different points along its route,
and by a variety of diseases (1).
The clinical description of oculosympathetic paresis was first described as long ago as 1727 where it was first noted as a complication during experimental intercostal nerve transections in dogs.
The syndrome takes its name from...
Findings and procedure details
Patients with disease of the oculosympathetic chain may present to the medical profession in a variety of different ways.
Acute neurological presentations include stroke,
trauma,
vascular dissection and some inflammatory diseases.
Alternatively,
patients with Horner’s syndrome may present to ophthalmology services or to medical specialties as new manifestations of established diagnoses,
for example tumour progression in known carcinoma.
The initial mode of radiological investigation is guided by the likely diagnosis.
Imaging in the acute setting is often with computed tomography (CT) of the brain +/-...
Conclusion
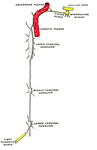
The oculosympathetic tract follows a long and circuitous anatomical course from its central location within the hypothalamus,
via the cervical spine and neck,
to its distal innervation within the orbit.
The function of the oculosympathetic pathway can be disrupted at any point along its course by a variety of different pathologies.
Knowledge of the anatomy of the pathway and understanding of the disease processes affecting the first,
second and third order neurones within the pathway aids the reviewing radiologist to identify the site of disease...
Personal information
Dr Lucy Childs.
The Royal London Hospital,
Department of Clinical Radiology,
Barts Health,
London,
UK.
[email protected]
References
Lee,
JH et al.
Neuroimaging Strategies for Three Types of Horner Syndrome with Emphasis on Anatomic Location.
Neuroradiology.
AJR:2007;188:W74-W81.
<http://www.whonamedit.com/synd.cfm/1056.html> [Accessed 21/12/13]
George,
A.
Haydar,
AA.
Adams WM.
Imaging of Horner’s syndrome.
Clinical Radiology.
2008;63:499-505.
Bardorf,
C.
Horner Syndrome.
Medscape.http://emedicine.medscape.com/article/1220091-overviewLast accessed 20/12/13.
Guerrero,
M.
Pancoast Tumour Imaging.
http://emedicine.medscape.com/article/359881-overview.
Last accessed 20/12/13
Lance JW,
Drummond PD,
Gandevia SC,
Morris JG.
Harlequin syndrome: The sudden onset of unilateral flushing and sweating.
J Neurol Neurosurg Psychiatry.
1988 May;51(5):635-42.
Walton KA,
Buono LM,
Horner syndrome,
Curr Opin Ophthal 2003;14:357-363....