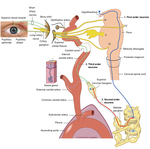
Patients with disease of the oculosympathetic chain may present to the medical profession in a variety of different ways.
Acute neurological presentations include stroke,
trauma,
vascular dissection and some inflammatory diseases.
Alternatively,
patients with Horner’s syndrome may present to ophthalmology services or to medical specialties as new manifestations of established diagnoses,
for example tumour progression in known carcinoma.
The initial mode of radiological investigation is guided by the likely diagnosis.
Imaging in the acute setting is often with computed tomography (CT) of the brain +/- CT imaging of the neck and CT angiography of carotid or intracranial vessels.
Further delineation with magnetic resonance imaging (MRI) is common.
MRI circumvents the beam hardening artifact seen on CT within the posterior fossa and adjacent to the temporal bones and provides excellent soft tissue contrast and spatial resolution.
Plain radiography or CT imaging of the chest is valuable where Pancoast tumours are suspected,
or in known lung carcinoma or trauma.
MRI T1-weighted imaging with gadolinium enhancement are useful for highlighting neoplastic and some inflammatory processes.
Standard T2-weighted imaging is typically performed,
along with fluid attenuated inversion recovery sequences (FLAIR),
diffusion-weighted imaging is particularly helpful in the setting of acute stroke (1,
3).
Ultrasound is useful in some clinical scenarios to identify disease within the soft tissues of the neck.
Supraclavicular lymphadenopathy and other masses within the neck may be visualised using ultrasound and provide guidance when obtaining cytological samples for diagnosis.
Below we present a series of radiological examples of disease affecting the oculosympathetic pathway.
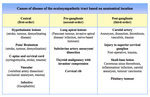
Cases are discussed based on site of disruption to the pathway; from central,
preganglionic to postganglionic.
Central disease of the oculosympathetic pathway
Case 1
This 70 year old man underwent imaging investigations as part of a screen for deteriorating cognition.
Two years previously he had presented acutely to hospital with ataxia,
dysarthria,
nystagmus,
quadraparesis and Horner’s syndrome (Fig. 4).

Fig. 4: Axial FLAIR MRI sequence. Area of focal gliosis in the right pontomesencephalic region resulting from thrombosis of the basilar artery and associated perforators.
An MRI brain performed during the acute admission demonstrated an area of abnormal signal centred in the right pontomesencephalic region.
The axial FLAIR MRI features (Fig. 4) are in keeping with an established area of gliosis.
These appearances are the result of previous thrombosis within the basilar artery and associated perforators.
The patient’s Horner’s syndrome was caused by disruption to central fibres of the oculosympathetic chain as they descend caudally within the brainstem.
Central disruption to first order fibres is most commonly due to infarction.
As detailed in Table 2 other causes of disruption include tumour,
inflammatory processes and traumatic injuries.
Wallenberg's syndrome or 'lateral medullary syndrome' is caused by thrombosis of the posterior inferior cerebellar artery (PICA). The vascular territory affected in our case did not correspond to the PICA distribution.
However,
Wallenberg's syndrome represents a well recognised presentation of acute vascular injury to the central oculosympathetic tract.
The typical presentation is: nystagmus,
dysphagia,
slurred speech,
ataxia,
vertigo,
Horner’s syndrome,
unilateral facial numbness and contralateral loss of pain and temperature sensation.
Case 2
This 73 year old man presented with acute onset of ophthalmoplegia with a right Horner’s syndrome,
nystagmus,
ataxia,
dysarthria and a partial third cranial nerve palsy.

Fig. 5: Axial T2W MRI sequence. There is abnormal increased T2 signal affecting predominantly the tegmentum of the pons with a more focal discrete area of signal change in the right side of the posterior tegmentum.
In this image (Fig. 5) from the Axial T2W MRI sequence abnormal increased T2 signal is seen predominantly affecting the tegmentum of the pons,
with a more focal,
discrete area of signal change in the right side of the posterior tegmentum.
Fig. 6 is a cross section from the B1000 Diffusion weighted MRI which demonstrates a focus of restricted diffusion within the posterior tegmentum of the pons.
Reduced signal can be seen on the corresponding ADC at this site.
These features are consistent with an acute ischaemic insult.

Fig. 6: MRI B1000 Diffusion weighted imaging demonstrates a focus of restricted diffusion within the posterior tegmentum of the pons. There was corresponding reduced signal on the ADC at this site consistent with an acute ischaemic insult.
Although not a complete set of symptoms the clinical picture is again suggestive of lateral medullary syndrome.
The imaging supports disruption of the central first order oculosympathetic fibres as they traverse the midbrain.
Case 3
This 39 year old man presented with acute onset of left sided Horner’s syndrome associated with a 7 day history of headache.

Fig. 7: Axial contrast enhanced CT. There is a heterogeneously enhancing tumour invading the left side of the thalamus with associated obstructing hydrocephalus. This was proven to be a high grade glioma on histological sampling.
Fig. 7 and Fig. 8 are cross sections from axial contrast enhanced CT imaging of the brain.
There is a heterogeneously enhancing tumour invading the left side of the thalamus with associated obstructing hydrocephalus.
This was proven to be a high grade glioma on histological sampling.

Fig. 8: Axial contrast enhanced CT. As above, heterogeneously enhancing tumour invading the left side of the thalamus with associated obstructing hydrocephalus, histologically found to be a high grade glioma.
The Horner’s syndrome in this case again results from disruption of the central first order oculosympathetic fibres traversing the brainstem.
Case 4
This 70 year old lady had progressive decline in her visual acuity over 6 months.
She had a shorter 3-4 week history of right sided eyelid droop which precipitated her presentation to hospital.
On examination she had a constricted right pupil,
right sided ptosis and bitemporal hemianopia (Fig. 9).

Fig. 9: Post contrast CT sagittal reconstruction images clearly demonstrate a large mass in the pituitary fossa with superior extension into the hypothalamus and features of bony skull base invasion. This was an invasive pituitary macroadenoma.
A large mass can be visualised within the pituitary fossa with superior extension into the hypothalamus and features of bony skull base invasion.
The axial image Fig. 10 demonstrates tumour surrounding the right internal carotid artery. The imaging appearances correspond to an invasive pituitary macroadenoma.

Fig. 10: Axial post contrast CT images centred on the pituitary fossa of the same patient demonstrate tumour surrounding the right internal carotid artery.
This case is discussed as a ‘central’ cause of Horner’s syndrome due to invasion of the hypothalamus.
However, the ocular Horner's signs may also result from disruption of post-ganglionic oculosympathetic fibres surrounding the internal carotid artery.
In this location the proximal and distal fibres of the oculosympathetic pathway are in close proximity.
The patient did not have loss of sweating on the ipsilateral side of the face which is anatomically suggestive of a distal site of disruption.
Pre-ganglionic disease of the oculosympathetic pathway
Preganglionic disease of the oculosympathetic pathway may result from: cervical disc herniation,
primary neurogenic tumours (paragangliomas),
nerve sheath tumours (schwannomas),
traumatic nerve avulsion or penetrating injuries. Iatrogenic injury to the tract is well recognised and may occur after neck dissection,
anaesthetic nerve blocks or intercostal drain insertion.
Aneurysmal dilatation or dissection of the subclavian artery may disrupt the pathway.
Similarly,
masses within the neck such as bulky thyroid disease or lymphadenopathy can affect the tract in its preganglionic portion (Table 2).
Pancoast tumours are primary malignancies of the lung affecting the pleuropulmonary groove (pulmonary sulcus).
Pancoast tumours have a well established association with Horner’s syndrome and are often one of the first differentials considered by doctors and medical students alike.
In this clinical circumstance the resultant Horner’s syndrome usually results from invasion of the stellate ganglion.
Inferior fibres of the brachial plexus may be affected by Pancoast tumours.
This causes pain in the ipsilateral arm and shoulder with paraesthesia on the same side (3,5).
Examples of pre-ganglionic disease of the oculosympathetic pathway are demonstrated below.
Case 5
This 44 year old woman had subacute onset of left sided Horner’s syndrome.
She had a history of intermittent sensory and motor symptoms in her right arm and leg although had not previously sought medical help.

Fig. 11: Sagittal T2W MR Images reveal foci of high T2 signal within the cervical and thoracic cord.
The sagittal (Fig. 11) and axial (Fig. 12) T2W MR images demonstrate multiple foci of high T2 signal within the cervical and thoracic cord. MRI sequences of the brain demonstrated further foci of high signal in the peri-ventricular deep white matter and confirmed the suspected diagnosis of demyelinating disease. Oligoclonal bands in the cerebrospinal fluid and the relapsing-remitting clinical course of the disease established the diagnosis as multiple sclerosis.

Fig. 12: Post contrast axial T1W MRI images demonstrate further foci of high signal within the cervical spine in keeping with an active plaque of demyelination.
The focus of high signal seen on the sagittal CT reformat of the cervical cord is the site of synapse between the central and preganglionic fibres of the oculosympathetic pathway,
the ‘cilispinal centre of Budge.’ Fibres leave the cord at the T1 level and ascend within the neck.
Demyelination of pre-ganglionic fibres was the cause of this patient's Horner’s syndrome.
Demyelinating disease can affect the oculosympathetic chain at any point along its length from its central origin to the distal post-ganglionic portion.
Case 6
This 48 year old man underwent C6-C7 discectomy and fusion.
He developed sudden onset right Horner’s syndrome 24 hours post surgery.

Fig. 13: This sagittal contrast enhanced CT demonstrates a focal soft tissue mass anterior to the C7/T1 operative site. This relates to a haematoma within the right pre-vertebral space.

Fig. 14: The small right pre-vertebral haematoma is visualised on axial CT.
Sagittal (Fig. 13) and axial (Fig. 14) contrast enhanced CT images of the neck demonstrate a focal soft tissue mass anterior to the C7/T1 operative site.
This relates to a haematoma within the right pre-vertebral space.
The visualised haematoma is compressing second order oculosympathetic fibres as they ascend within the neck after leaving the cervical spine.
This compression induced right sided Horner's syndrome.
The patient was managed conservatively,
and symptoms gradually resolved.
Case 7
This 73 year old man presented with left arm weakness,
areflexia and left Horner’s syndrome.
He had an established diagnosis of small cell carcinoma of the left lung.

Fig. 15: MRI axial T1WI demonstrates metastatic nodal disease in the left supraclavicular fossa, some of which is also intimately related to the cords of the brachial plexus.
The axial (Fig. 15) and coronal (Fig. 16) T1W MR images demonstrate metastatic nodal disease in the left supraclavicular fossa,
some of which is also intimately related to the cords of the brachial plexus.
The primary lung carcinoma can be visualised at the left hilum in the coronal image.

Fig. 16: Coronal post contrast T1W MR image. Necrotic, metastatic lymphadenopathy is seen in the root of the neck. The primary small cell lung carcinoma is visualised at the left hilum in this coronal image.
Pancoast tumours typically induce Horner's syndrome by invasion of the stellate ganglion.
Arm weakness,
pain and paraesthesiae occur when inferior cords of the brachial plexus are also involved.
In this case bulky metastatic lymphadenopathy within the neck is compressing the stellate ganglion and cords of the branchial plexus disrupting the oculosympathetic pathway.
Case 8
This 52 year old lady presented with a palpable right-sided neck mass and a right Horner’s syndrome.
The mass had been gradually enlarging over many months.

Fig. 17: Coronal contrast enhanced CT demonstrates a large right inferior neck mass lying deep to the right lower pole of the thyroid gland. This was found to be a follicular thyroid neoplasm.
Multinodular change was evident within the thyroid gland,
however a mass related to the inferior aspect of the gland extends deep into the neck (Fig. 17, Fig. 18).
The lesion lies in the anatomical region of the stellate ganglion and induced a right sided Horner’s syndrome.

Fig. 18: MRI sagittal T2WI demonstrates a mass arising from the posterior aspect of the lower pole of the right thyroid gland.
Nerve sheath tumours such as schwannomas may also present in this anatomical location and present with a similar clinical presentation.
Case 9
This 15 year old girl had an 8 year history of right sided facial sweating and flushing.

Fig. 19: Axial T2W MRI demonstrates an ovoid mass at the level of the right carotid bifurcation. The mass splays the bifurcation and displaces the internal carotid artery medially.

Fig. 20: T2W sagittal MRI imaging depicts the ovoid mass in the region of the superior cervical ganglion. This was a nerve sheath tumour causing Harlequin syndrome.
Axial (Fig. 19) and sagittal (Fig. 20) T2W MR images readily demonstrate a soft tissue mass near the superior cervical ganglion.
The lesion was felt to represent a nerve sheath tumour based on MR appearances.
An ultrasound guided fine needle aspiration of the lesion was performed for cytological analysis.
This confirmed the suspected diagnosis of nerve sheath tumour.
Second order fibres of the oculosympathetic tract ascend in close proximity to the internal and external carotid arteries.
Fibres following the course of the external carotid artery innervate smooth muscle within the facial sweat glands. Harlequin syndrome is caused by compromise of vasomotor and sudomotor sympathetic fibres that supply the face.
It causes facial flushing and sweating contralateral to the side of the lesion.
It is not certain why this overreaction occurs,
but is presumably a compensatory mechanism (6).
Anhydrosis occurs on the ipsilateral side of the face.
Horner’s syndrome may be present on the affected side.
Our case is not entirely typical of Harlequin syndrome as facial flushing and sweating occurred on the same side as the tumour.
Post-ganglionic disease of the oculosympathetic pathway
Postganglionic,
third order neurons of the oculosympathetic tract extend from the superior cervical ganglion to the orbit.
The carotid bifurcation,
skull base and cavernous sinus are closely associated with the ascending fibres.
Damage to the postganglionic oculosympathetic pathway is more commonly associated with facial pain.
Trauma is the most common cause of disruption at this level.
Carotid artery dissection is another commonly implicated pathology.
Postganglionic Horner’s syndrome is categorised into three subsections: disease of the internal carotid artery,
disease at the level of the skull base,
and disease of the cavernous sinus or orbital apex (7).
If cranial nerves III,
IV,
V or VI are impaired,
this suggests the site of pathology may relate to the cavernous sinus or superior orbital fissure.
Loss of sight suggests the orbital apex with compromise of the optic nerve (1).
Case 10
This 81 year old man underwent radical resection of a T1N2M0 squamous cell carcinoma of the tongue base in 2011.
He had flat reconstruction and radiotherapy.
He represented 2 years post-op with a new left sided Horner’s syndrome.

Fig. 21: Axial contrast-enhanced CT of the neck demonstrates soft tissue encasement of the internal carotid artery by recurrent extra nodal SCC.
The axial contrast enhanced CT images (Fig. 21) demonstrate ill-defined,
soft tissue adjacent to the left carotid sheath.
New pulmonary nodules were also visualised within the lung parenchyma on CT.
This was histologically confirmed to be recurrent squamous cell carcinoma with pulmonary metastases.
Soft tissue encasing the carotid sheath is closely apposed to the carotid plexus of the oculosympathetic pathway.
The Horner's syndrome in this case most probably relates to fibre compression or invasion at this site.
Facial sweating was typically unaffected as lesions affecting distal oculosympathetic fibres will not cause facial anhydrosis.
This is because sweat glands are supplied by fibres exiting proximal to this point in the pathway.
Case 11
This 38 year old man presented to the vascular surgeons with a palpable,
pulsatile mass in the right anterior triangle of his neck.
On examination he was noted to have a mild right sided ptosis and anisocoria.
In 1993 he was accidentally shot in the neck with a pellet gun.
He underwent emergency surgery and neck soft tissue reconstruction.
Further surgery was performed in 2003 to remove a residual pellet.
CT angiography of the neck revealed the clinically palpable mass related to an ectatic portion of the proximal right internal carotid artery.
Importantly,
a 1.7cm partially thrombosed,
peripherally calcified pseudoaneurysm of the distal right internal carotid artery was incidentally visualised (Fig. 22, Fig. 23).

Fig. 22: Axial CT angiogram just above the carotid bifurcation demonstrates post traumatic pseudoaneurysm of the right proximal ICA (long arrow) and an adjacent bullet fragment (arrow head).
Traumatic penetrating injuries can cause direct vascular injury or vascular inflammation.
Arterial injury can lead to pseudoaneurysm formation and compression of adjacent structures.
The right sided ptosis and anisocoria were due to compression of oculosympathetic fibres by the right internal carotid artery pseudoaneurysm.

Fig. 23: Coronal contrast enhanced CT of the neck demonstrates a peripherally calcified, partially thrombosed pseudoaneurysm of the right internal carotid artery.
Case 12
This 46 year old man presented to his general practitioner with progressively worsening left sided ptosis,
he was otherwise well.
Clinical examination revealed a left sided Horner’s syndrome.

Fig. 24: Contrast enhanced axial CT reveals a low attenuation mass at the level of the skull base. This lesion was found to be a sympathetic nerve sheath tumour.
Contrast enhanced axial CT (Fig. 24) reveals a low attenuation mass at the level of the skull base.
The lesion is closely related to the left carotid plexus of the oculosympathetic chain.
Compromise of these fibres caused the left sided Horner's syndrome.
The mass was a sympathetic nerve sheath tumour (Fig. 25).

Fig. 25: Sagittal contrast enhanced CT of the neck demonstrates a sympathetic nerve sheath tumour at the level of the skull base.
Case 13
This 39 year old man presented for further investigation to the ear,
nose and throat surgeons with a 4-month history of conductive deafness.
On examination he had a retracted tympanic membrane,
partial ptosis and pupillary miosis.

Fig. 26: High resolution non contrast CT of the temporal bones reveals an expansile mass within the right petrous apex. The epicentre is focused on the carotid canal. Associated bone remodelling is visualised.
High resolution bone reformats of the temporal bones (Fig. 26) reveal an expansile mass within the right petrous apex.
The epicentre is focused on the carotid canal.
The mass compromised the right eustacian tube with resultant opacification of the entire middle ear cavity and mastoid air cells.
Associated bone remodelling is well visualised and suggests a slowly progressive process.
Aneurysmal dilatation of the internal carotid artery was suspected based on these appearances and a CT angiogram of the intracranial vessels was performed (Fig. 27).

Fig. 27: CT angiogram of the intracranial vessels demonstrates aneurysmal dilatation of the right internal carotid artery within the carotid canal.
The intracranial CT angiogram demonstrates fusiform aneurysmal dilatation of the right internal carotid artery related to the carotid canal.
The case was discussed in the neurosurgical multi-disciplinary team meeting.
Catheter angiography confirmed an intact circle of Willis.
Decision was made to sacrifice the right internal carotid artery due to significant risk of aneurysm rupture into the adjacent sphenoid sinus.
The aneurysm was embolised by interventional neuroradiologists.
Post-embolisation appearances are demonstrated in Fig. 28.

Fig. 28: T2W MRI demonstrates the post embolisation appearances of the internal carotid artery aneurysm.
Case 14
This 66 year old man presented with sudden onset left sided Horner’s syndrome associated with left sided facial pain.

Fig. 29: Axial T2W MRI demonstrates dissection of the left internal carotid artery with pseudoaneurysmal dilatation of the vessel.
Axial T2W MRI (Fig. 29) and the axial source 3D Time Of Flight MR angiogram (Fig. 30) demonstrates dissection of the left internal carotid artery with pseudoaneurysmal dilatation of the vessel.
Dissection,
pseudoaneurysm,
trauma or inflammation of arteries adjacent to the oculosympathetic chain can interfere with sympathetic supply to the orbit.
This may manifest clinically with Horner's syndrome as in this case.

Fig. 30: Axial source 3D Time Of Flight MR angiogram. There is dissection of the left internal carotid artery with associated pseudoaneurysmal dilatation.
At the level of the skull base the carotid artery is susceptible to traumatic injury.
Patients with connective tissue diseases such as Ehlers-Danlos syndrome or fibromuscular dysplasia are more susceptible to spontaneous vascular dissection (8).
Case 15
This 56 year old man presented to hospital with headache,
vomiting and diplopia.
He had an established diagnosis of poorly differentiated metastatic neuroendocrine tumour.
On examination he had right sided Horner’s syndrome,
and impaired adduction of the right eye.
Oculomotor nerve compromise was suspected,
the remaining cranial nerves were intact.
Cross-sectional CT imaging was performed to look for an intracranial aetiology (Fig. 31).

Fig. 31: Contrast enhanced axial CT of the brain reveals a heterogenously enhancing mass within the right cavernous sinus.
Contrast enhanced axial CT of the brain (Fig. 31) reveals a heterogenously enhancing mass within the right cavernous sinus.
An MRI of the brain was performed (Fig. 32).

Fig. 32: Coronal post contrast T1W MR at the level of the cavernous sinus clearly demonstrates heterogenously enhancing soft tissue within the right cavernous sinus. The cavernous portion of the internal carotid artery is encased although not occluded by tumour. This is a deposit from the metastatic neuroendocrine tumour.
Patients with Horner's syndrome associated with impairment of cranial nerves III,
IV,
V and VI suggest the cavernous sinus or superior orbital fissure as the site of pathology.
This patient experienced Horner's syndrome associated with impairment of the oculomotor cranial nerve.
The soft tissue disrupting the oculosympathetic pathway within the cavernous sinus was a metastatic deposit from the neuroendocrine tumour.