Epidemiology
Astrocytic tumors are the most common brain tumors of childhood,
comprising approximately 20% of all childhood malignancies and more than half of all primary CNS malignancies.
Most cases occur in the first decade of life,
with the peak incidence occurring in children aged 5-9 years.
High-grade supratentorial tumors occur slightly later,
with a median age at diagnosis of 9-10 years.
The term "astrocytoma" contains numerous tumors that differ by location,
morphological characteristics,
the degree of invasiveness,
growth rate,
tendency to progression and clinical course.
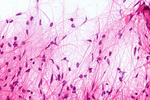
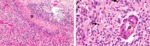
Pathomorphology
Astrocytomas are the most common glial tumors arising from astrocytes. This type of tumors does not usually spread outside the brain and spinal cord and it does not usually affect other organs; they can occur in most parts of the brain and occasionally in the spinal cord.
Astrocytomas can be divided into two large groups:
1.
Diffuse form (mostly high grade)
- low grade astrocytoma: WHO grade II (10-15% of astrocytomas)
-
- fibrillary astrocytoma
- protoplasmic astrocytoma
- gemistocytic astrocytoma
- anaplastic astrocytoma: WHO grade III (25% of astrocytomas)
- glioblastoma multiforme: WHO grade IV (50-60% of astrocytomas)
- giant cell glioblastoma: WHO grade IV (rare)
- gliosarcoma: WHO grade IV (rare)
- gliomatosis cerebri
2.
Localized form (mostly have lower grade)
- pilocytic astrocytoma: WHO grade I
- pilomyxoid astrocytoma: WHO grade II
- subependymal giant cell astrocytoma: WHO grade I
- pleomorphic xanthoastrocytoma: WHO grade II
Clinical presentation
Presenting symptoms for childhood astrocytomas depends on:
- location;
- Size of the tumor;
- Rate of tumor growth;
- Chronology and age of the child.
Astrocytomas can be asymptomatic for a long time and may clinically manifested with increased intracranial pressure,
headaches,
movement disorders,
hemiparesis,
seizures (40-50% of cases),
speech disorders and other focal symptoms.
Treatment options of astrocytomas depends on their anatomic location,
biologic aggressiveness and age of the patient.
It is typically complex,
combining the maximum possible surgical resection of the tumor,
followed by radiation therapy and chemotherapy in a number of cases (depending on the histological subtype of the tumor).
Prognosis
Children with low-grade tumors have a relatively favorable prognosis,
especially when the tumors can be completely resected.
Children with high-grade tumors generally have a poor prognosis,
unless the tumor is an anaplastic astrocytoma that can be completely resected.