Stages of lymphoma were distributed as follows: stage I - 5 patients,
II - 28,
III - 21,
IV - 35.
The number of ChT courses was from 3 to 8. Additional treatment after PET/CT was performed in 46 (52%) patients,
including 20 with LH and 26 with NHL.
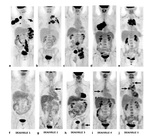
Examples of the establishment of Deauville categories 1-5 are shown in Figure 1.
First of all,
in the analysis of PET/CT images,
the foci of physiological and non-tumor 18F-FDG accumulation were excluded.
The exact differentiation was difficult in some cases.
Thus,
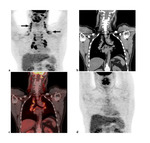
in two (2%) patients the category D 5 was prospectively and retrospectively established on the basis of increased uptake of 18F-FDG (SUV 8.9 and 13.7) in the mediastinal and hilar lymph nodes,
but later sarcoidosis was verified (Fig.
2).
For sarcoidosis associated with lymphoma the symmetrical involvement of mediastinal and hilar lymph nodes is characteristic,
with persistent high metabolic activity after ChT despite regression of other lesions.
Diffuse increased accumulation of 18F-FDG in the bone marrow above the liver was noted in 7 (8%) patients.
Lymphoma recurrence developed in 2 out of 7 people.
Deauville categories assigned by different doctors coincided in 85% of cases (coefficient of agreement κ 0.80),
lymphoma response category – in 97% (κ 0.92).
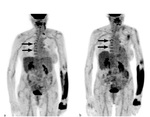
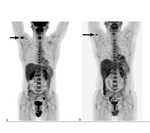
Exemplary cases in which there was a discrepancy in the establishment of Deauville categories are shown in Figures 3 and 4.
Prognostic properties of Deauville scale
The diagnostic efficacy of PET/CT is shown in Table 1.
A rather low prognostic value of positive PET/CT result in the diagnosis of progression/relapse within 6 months was noted.
It varied from 36% in patients who received additional treatment to 73% in patients who didn’t receive additional treatment.
The reasons for low positive prognostic value (PPV) are false positive PET/CT findings.
One-year progression-free survival (PFS) in categories D 1-2 was 95%,
D 3 — 57%,
D 4-5 — 56%.
PFS for categories D 3 and D 4-5 did not differ significantly (p= 0.52).
Semi-quantitative analysis of PET/CT
Metabolically active non-physiological foci with uptake above the mediastinal blood pool were detected after completion of ChT in 40 (45%) of 89 patients.
Progression/relapse of lymphoma developed in 19 (48%) of 40 patients during observation time.
SUV of metabolically active residual lesions > 4.7 predicts lymphoma progression/recurrence with sensitivity of 68% and a specificity of 81% (p=0,0001).