Keywords:
Interventional non-vascular, Biliary Tract / Gallbladder, Fluoroscopy, Drainage, Cholangiography, Multidisciplinary cancer care
Authors:
D. G. Castiglione1, C. Gozzo1, L. Mammino2, F. Midiri1, G. Caltabiano3, S. Palmucci2, A. Basile2; 1Palermo/IT, 2Catania/IT, 3CATANIA (CT)/IT
DOI:
10.26044/ecr2019/C-0132
Aims and objectives
Percutaneous Transhepatic Biliary Drainage (PTBD) is an established image-guided procedure which leads to the drainage of the obstructed bile duct system.
PTBD main indications include decompression of intra and extrahepatic biliary ducts in case of malignant or benignant obstruction,
cholangitis,
the decrease serum bilirubin before starting chemotherapy,
biliary stent placement [1-3].
Given the main palliative nature of PTBD,
it is obvious that besides survival benefits,
Health-Related Quality of Life aspects should represent a crucial point.
After the PTBD,
the relief of obstructive symptoms,
especially pain and pruritus,
and the improvement of liver functions,
have a positive impact on QoL [4].
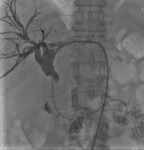
The choice of right or left side approach to perform biliary puncture and position drainage catheter is debated [5-12].
The right approach is often adopted because many interventional radiologists are more comfortable with the technique and the right lobe contains most of the hepatic parenchyma,
but the left side approach has also advantages,
it allows favourable angles for catheterization and is less uncomfortable than intercostal right placement (Fig 1).
We have focused our attention on the Quality of Life in patients who underwent PTBD from right or left access,
utilizing a structured questionnaire,
the “EORTC QLQ-BIL21”,
developed by the European Organisation for Research and Treatment of Cancer (EORTC),
and designed for use among patients with cholangiocarcinoma and gallbladder cancer,
that could be well-suited in the evaluation of Quality of Life in patients who undergo PTBD [13].
Therefore,
our purpose was to investigate differences in terms of Quality of Life in patients who underwent PTBD via right or left access,
when both accesses are feasible,
using a standardized structured questionnaire like the “EORTC QLQ-BIL21”(Tab 1).