Keywords:
Interventional non-vascular, Biliary Tract / Gallbladder, Fluoroscopy, Drainage, Cholangiography, Multidisciplinary cancer care
Authors:
D. G. Castiglione1, C. Gozzo1, L. Mammino2, F. Midiri1, G. Caltabiano3, S. Palmucci2, A. Basile2; 1Palermo/IT, 2Catania/IT, 3CATANIA (CT)/IT
DOI:
10.26044/ecr2019/C-0132
Conclusion
The purpose of this study was to compare Quality of Life in patients who underwent PTBD via right versus left access when both accesses were feasible.
Our results showed highly significant difference related to pain,
reported higher in patients who underwent PTBD via right access (p< 0.001).
The continuous stimulation of intercostal nerves could play a crucial role,
and the additional independent questions about localizing pain confirm that intercostal pain is the main localization when the PTBD is performed via right access (Tab 4).
Respiratory continuous discomfort could influence the higher registered level of tiredness and anxiety in patient with PTBD via right access because the EORTC QLQ-BIL21 "Anxiety" and "Tiredness" scales showed a highly significant difference (p< 0.01) between subgroups A and B.
Patients with drainage catheter on the right side showed significant difficulties in the management of tubes and bags,
“Drain scale” value p< 0.05.
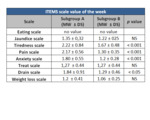
When comparing symptoms relief as jaundice or pruritus or weight loss no statistical difference was shown,
demonstrating the effectiveness of the PTBD either via right or left access (Tab 5).
In conclusion,
our study showed that the choice of left access for PTBD results in better QoL for patients,
with a reduction of pain,
tiredness,
anxiety and better management of catheter drainage.
As QoL is considered a "hard endpoint" by ASCO,
we hope the results of this study could influence decisions in tumour boards in order to provide better QoL for patients with malignant obstructive jaundice [19].