Keywords:
Abdomen, Contrast agents, Pancreas, CT-Quantitative, Experimental investigations, Treatment effects, Cancer
Authors:
T. H. Perik, E. Van Geenen, E. J. Smit, L. A. A. Brosens, M. W. J. Stommel, E. C. Gootjes, K. J. H. M. Van Laarhoven, H. Huisman, J. J. Hermans; Nijmegen/NL
DOI:
10.26044/ecr2021/C-14092
Conclusion
The major finding in this study was that percentual change in blood flow was higher in patients who responded to chemotherapy.
A possible explanation for increased blood flow is that treatment slows down extracellular matrix accumulation in the tumor, allowing improved perfusion.[6]
After neoadjuvant chemotherapy current staging tools (RECIST) often underestimate treatment response. More accurate restaging can improve selecting patients for R0-resection (resection margin free of tumor) and prevent futile surgery. Earlier response assessment for palliative chemotherapy could help in preventing unnecessary toxicity for non-responders, possibly reducing morbidity.
At baseline we did not see significant differences in blood flow for our population. Differences at baseline would help in selecting patients who benefit from chemotherapy.
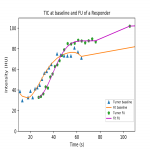
This is an early result of a prospective study, therefore the number of patients (n=12) is still limited and no correlation with overall survival or pathological grading of response was possible yet. The advantage of an interleaved scan is that in a ‘one stop shop’ protocol both diagnostic and functional information is obtained. Adding no extra scan time and using a single contrast injection. Delineation of PDAC on a CECT is often difficult and therefore defining a ROI is difficult. Current analysis is performed in one slice, 3D tumor analysis could improve the reliability of perfusion parameters.
Our results show that perfusion parameters contain valuable information concerning treatment assessment. However future work is needed on this novel analysis to increase stability and make the step towards implementation into clinical practice. Current kinetic models show a high variance in perfusion parameters making it difficult to compare results between investigators.[7]
Conclusion: Change in perfusion parameters obtained using an interleaved CTP protocol, might be a valuable functional biomarker to evaluate response to chemotherapy in patients with PDAC.



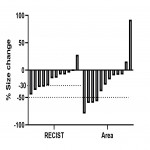

![Fig 6: Percentual change in blood flow (BF) after chemotherapy in responders [R] and non-responders [NR]. Categorized by the RECIST-criteria (p=0,972) and Area (p=0,024).](https://epos.myesr.org/posterimage/esr/ecr2021/158239/media/901820?maxheight=150&maxwidth=150)
![Fig 7: Percentual change in maximum enhancement after chemotherapy in responders [R] and non-responders [NR].](https://epos.myesr.org/posterimage/esr/ecr2021/158239/media/901821?maxheight=150&maxwidth=150)
