Congress:
EuroSafe Imaging 2021
Keywords:
Management, Oncology, Radioprotection / Radiation dose, CT, Audit and standards, Cost-effectiveness, Health policy and practice, Cancer, Outcomes, Patterns of Care
Authors:
I. RAJENDRAN, L. Tandon
DOI:
10.26044/esi2021/ESI-11271
Conclusion
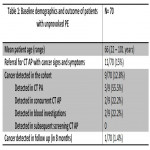
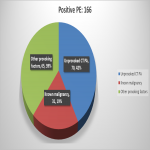
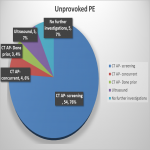
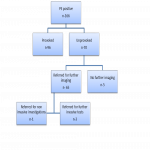
Majority of cancer in the study cohort was detected in the CT PA examination and also some were detected in concurrent CT AP. The cancer detection rate on CT AP done following unprovoked PE to look for occult cancer was low, which is lower than other established studies (2.3%, 5.06%). This could be due to limitations by smaller data and not including Deep venous thrombosis (DVT) patients in the audit, although the NICE guidelines included both DVT and PE. Another limitation is that mammograms were not included as our institute is not a screening centre. Further extensive investigations such as CT AP in patients without signs and symptoms of cancer did not increase the frequency of cancer diagnosis. However, the presence of cancer does increase the chance of getting VTE as proved in our audit by the cancers diagnosed during the CT PA examination and in the setting where concurrent scans were done due to presence of clinical signs and symptoms. Following the audit, the radiology department of our institution agreed not to offer further CT abdomen and pelvis in patients with unprovoked PE without clinical signs and symptoms of cancer. This will essentially reduce unnecessary stress, anxiety and radiation exposure to patients.