Congress:
EuroSafe Imaging 2021
Keywords:
Management, Oncology, Radioprotection / Radiation dose, CT, Audit and standards, Cost-effectiveness, Health policy and practice, Cancer, Outcomes, Patterns of Care
Authors:
I. RAJENDRAN, L. Tandon
DOI:
10.26044/esi2021/ESI-11271
Purpose or learning objective
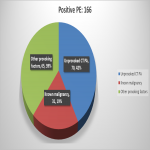
Venous thromboembolism (VTE) comprises of deep venous thrombosis (DVT) and pulmonary embolism (PE). This can be provoked by clinical risk factors such as recent major surgery, trauma, immobility, known malignancy, pregnancy or puerperium, smoking, obesity, underlying prothrombotic state or hormonal therapy. The term unprovoked DVT or PE is used when no such cause is identified (1).
There is an increased risk of cancer in people with unprovoked VTE, which can be undiagnosed at presentation. The diagnosis of cancer in such patients has implications that different agents and treatment durations preferred. Moreover, early identification of cancer is essential to maximise effectiveness (2). However, evidence shows no benefit from further investigations for occult cancer in the absence of signs or symptoms of cancer as the cancer detection rate mirrors that of the general population, which is approximately around 5 % (3). Hence, it is important that people should not be unnecessarily subjected to cancer investigations as these tend to be time-consuming, causes stress, anxiety and radiation exposure. This is the rationale behind recent update of NICE guideline in March 2020, which recommends reviewing the medical history and baseline blood test results and offering a physical examination without performing further cancer investigations unless they have relevant clinical symptoms or signs.
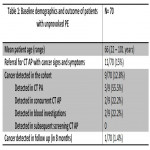
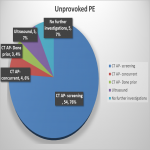
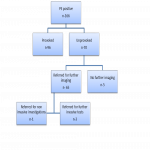
The aim of this audit is to determine imaging and pathological outcomes in patients with unprovoked PE referred for abdominopelvic computed tomography (CT) imaging. Identify the recommendations made on CT, their outcome and the cancer detection rate in these scans.